  
These include flat epithelial atypia, atypical ductal hyperplasia, and atypical lobular hyperplasia.ĭiagnostic investigations include obtaining a comprehensive history and clinical exam. Of the common fibrocystic breast changes, only proliferating lesions with atypia are associated with a clearly increased risk of breast cancer. After breast cancer treatment, 30% of women have persistent noncyclic mastalgia, especially those who are premenopausal, have a high body mass index, or have a concomitant psychological condition ( 6, e7).įibrocystic changes and risk of breast cancer In cases with no underlying pathology, rates of spontaneous remission within a few months to up to 3 years are high ( 5). 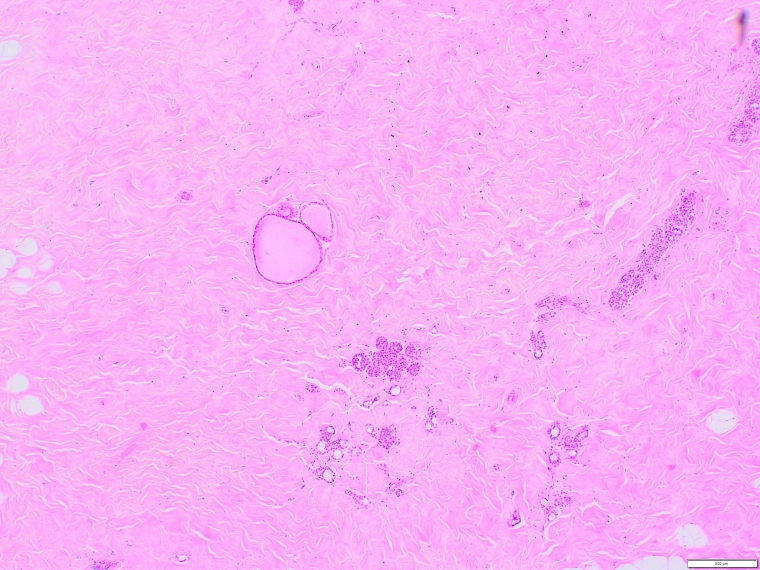
In a woman with noncyclic mastalgia, inflammatory, neoplastic, and vascular breast disease needs to be ruled out ( e6). The fact that cyclic mastalgia improves in association with hormonal changes such as when the menopause is reached, and during pregnancy and lactation, suggest a hormonal cause ( e5). Cyclic mastalgia manifests at around 30 years of age the onset of noncyclic mastalgia is notably later, at a mean age of 41. In two-thirds of cases, the pain is cyclic and is worst a week premenstrually and perimenstrually. Surveys have shown that more than half of all women report significant breast pain, which in 30% to 40% of cases impairs their everyday and sexual life ( e5). Differential diagnoses to rule out are chest pain of extramammary origin such as intercostal neuralgia and pain from cardiac or vertebrogenic causes. Mastalgia is classified as cyclic and noncyclic. Mastalgia (also called mastodynia) is the name given to pain related to the mammary gland occurring either spontaneously or in response to touch. Differential diagnoses for noncyclic mastalgia include inflammatory, neoplastic, and vascular breast disease. In two-thirds of cases, mastaliga is cyclic. Today’s minimally invasive techniques for achieving a confirmed histological diagnosis mean that surgical excision, previously common, can now be avoided in most cases. The BI-RADS (“breast imaging reporting and data system”) classification-the standardized description of radiological findings-offers the clinician recommendations for action ( table 2) ( 4). Typical presenting symptoms such as pain, a palpable mass, and nipple discharge can be caused by a wide array of benign differential diagnoses ( table 1) and require targeted diagnostic imaging in addition to a comprehensive history and clinical examination ( e4). The management of benign breast changes includes clinical, radiological, and if necessary histological diagnostic investigations to rule out malignancy palliation of symptoms and counseling and monitoring of patients at increased risk of breast cancer. Benign breast changes are more common in women of child-bearing age, peaking between the ages of 30 and 50, whereas the incidence of breast cancer peaks during the postmenopause ( e2, e3). Although breast cancer is detected in only 3% to 6 % of women with clinical symptoms, and in most cases the cause of the symptoms is benign, no evidence-based recommendations for the management of benign disease have been produced because the focus has been on the diagnosis and treatment of breast cancer ( 1, 3) ( e1). 
For this reason, breast changes are a cause of anxiety in patients and require a carefully targeted diagnostic process ( 2). At around 70 000 new cases a year, breast cancer is the most common form of cancer in women in Germany, occurring in approximately one in eight women at some time during their lives. According to data from the Netherlands and the USA, around 3% of women’s consultations with their general practitioners (GPs) are about breast symptoms ( 1, e1). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
